Nurse Manager Additions
 Ian took over leadership of the MICU on September 18. After honorably serving in the U.S. Marine Corps for six years, Ian earned his bachelor’s in nursing from East Carolina University. He then spent three years working in the Cardiac Care Unit in North Carolina before joining the Hopkins family as a nurse clinician and then a NCIII in the Department of Surgery in the Cardiovascular ICU (CVICU).
Ian took over leadership of the MICU on September 18. After honorably serving in the U.S. Marine Corps for six years, Ian earned his bachelor’s in nursing from East Carolina University. He then spent three years working in the Cardiac Care Unit in North Carolina before joining the Hopkins family as a nurse clinician and then a NCIII in the Department of Surgery in the Cardiovascular ICU (CVICU).
 Allison Olazo will become the nurse manager of the Progressive Cardiac Care Unit (Bloomberg 5 south) beginning October 2. Allison graduated with her bachelor’s in nursing from Rutgers University prior to starting her Hopkins career as a nurse in the PCCU. Through her commitment to nursing excellence, leadership and engagement, she has risen through the ranks in nursing leadership and went on to complete master’s degrees in nursing and business administration from Johns Hopkins University.
Allison Olazo will become the nurse manager of the Progressive Cardiac Care Unit (Bloomberg 5 south) beginning October 2. Allison graduated with her bachelor’s in nursing from Rutgers University prior to starting her Hopkins career as a nurse in the PCCU. Through her commitment to nursing excellence, leadership and engagement, she has risen through the ranks in nursing leadership and went on to complete master’s degrees in nursing and business administration from Johns Hopkins University.
Updates
On September 14, the DOM started a face-to-face team huddle in the command center. Charge nurses from all DOM units attend and report out expected discharges, admissions, staffing issues and barriers to discharge. Other attendees included in the huddle are: physical therapy, social work, case management, radiology, pharmacy and central bed management.
The Meyer building renovations are taking longer than expected. The move of Halsted 4 and H2O2 to the Meyer building will be December 14. The delay will affect all staff offices affiliated with these services.
A hospital-wide Central Line Associated Bloodstream (CLABSI) Infection prevention campaign kicked off in August. Every clinical area has named a champion who is receiving on-going training in policies, products and interventions to help reduce or prevent CLABSIs. Incidents of infections will continue to be discussed at unit-based CUSP meetings.
Family Involvement Menu
Patient centeredness is a key attribute of healthcare quality, which emphasizes the engagement of patients and families in care, decision-making and quality improvement. Patients admitted to the hospital are vulnerable to medical errors because of their sometimes limited ability to participate in clinical decision-making and to recognize and report adverse events. Engaging families in the care of patients has been suggested to improve the quality and safety of care.
In 2009, we designed and tested a Family Involvement Menu (FIM) in the WICU to improve family engagement in the care of their loved ones. The FIM is a one-page laminated document with a list of care activities (e.g., oral care, assist with ambulation, pillow repositioning) hung in each patient room. Families are invited and trained to perform any activities listed on the FIM. While the FIM is simple in concept, its implementation is a complex process requiring organizational readiness, keen understanding of the clinical workflow and adaptive changes to the work system. To address these challenges, we extended the FIM to a Family Involvement Program by including a series of educational activities and a structured approach to full implementation of the program.
The next phase of this work intends to implement the Family Involvement Program in other care areas and evaluate its impact on care processes (e.g., level of family engagement), patient outcomes (e.g., satisfaction) and employee outcomes (e.g., workload). We will guide individual units and facilitate collaboration across units through the implementation and evaluation process, which includes identifying needs of family engagement, adapting the FIM based on identified needs, implementing the Family Involvement Program and other work system changes and collecting data on the impact of the Family Involvement Program. It applies a collaborative approach, which emphasizes the involvement of different stakeholders (e.g., patients and families, clinicians) and the collaboration of different units in the adaptation and implementation of the Family Involvement Program.
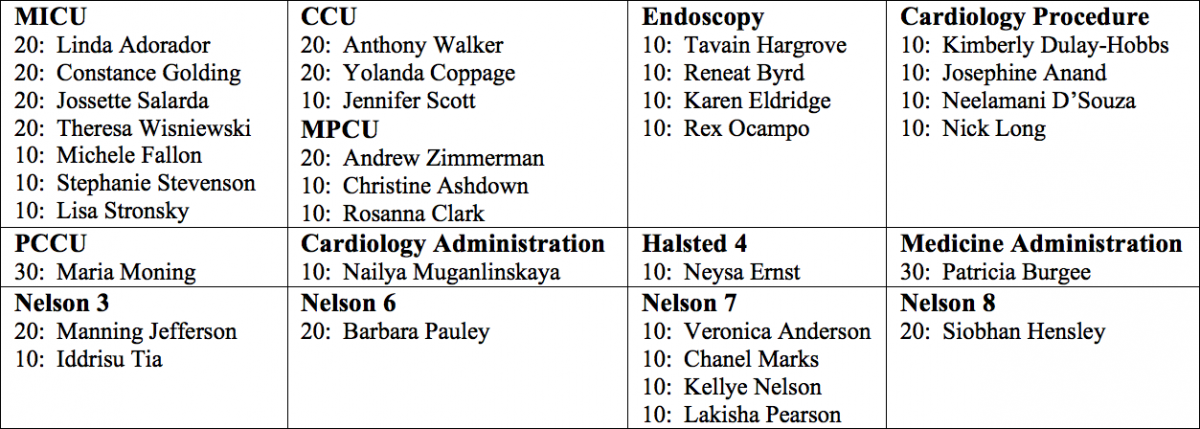
Congratulations and thank you to the following employees with 10 or more years of service:
All nurses in Bloomberg 5 south/PCCU: “Thank you for my life…I am eternally grateful for you all.”