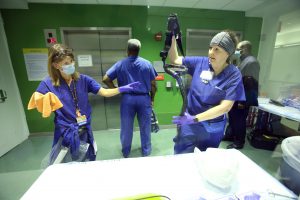
 No one is untouched by the COVID-19 pandemic. Although all departments in the School of Medicine and Johns Hopkins Health System have come together in remarkable ways to meet this challenge, no group has given more than the Department of Medicine. COVID-19 is fundamentally a medical illness, and our department is at the forefront in every aspect. Our nurses, residents, fellows, faculty and administrators are all involved and have substantially changed their work flow and, in many cases, their job descriptions to meet the demands of COVID-19. Each of our divisions has contributed in unique ways, addressing the clinical care, research and educational missions that are so critical to this response. With profound gratitude for these efforts, we are dedicating a series of brief reports to inform, thank and celebrate the contributions of these key divisions to our COVID-19 response.
No one is untouched by the COVID-19 pandemic. Although all departments in the School of Medicine and Johns Hopkins Health System have come together in remarkable ways to meet this challenge, no group has given more than the Department of Medicine. COVID-19 is fundamentally a medical illness, and our department is at the forefront in every aspect. Our nurses, residents, fellows, faculty and administrators are all involved and have substantially changed their work flow and, in many cases, their job descriptions to meet the demands of COVID-19. Each of our divisions has contributed in unique ways, addressing the clinical care, research and educational missions that are so critical to this response. With profound gratitude for these efforts, we are dedicating a series of brief reports to inform, thank and celebrate the contributions of these key divisions to our COVID-19 response.
Division of Cardiology:
- Members of the Division of Cardiology have effectively changed the way they see patients. Over 80 percent of outpatient visits are now telemedicine visits.
- Fellows and attendings are working side by side with pulmonary colleagues to care for patients with COVID-19 in the intensive care units.
- Cardiology researchers are studying the highly unusual cardiovascular complications of COVID-19, trying to understand the cause of inflammation and blood clots in these patients.
Division of General Internal Medicine:
- Telemedicine visits ramped up quickly, and members of GIM strategically reached out to high-risk patients to make sure they had access to what they needed. This included two faculty practices, the housestaff clinic at JHOC (Dr. Gail Berkenblit) and the After Care Clinic (Dr. Rosalyn Stewart), and the University Health Service (Dr. Spiro Marinopolous).
- Three faculty members secured a Hopkins Business of Health Initiative
- Dr. Jodi Segal “Rules-based approach to telemedicine triage”
- Drs. Jeremy Epstein and Case Overby Taylor “Will the Doctor see you now? An RCT of video vs. telephone primary care visits”
- Dr. Ben Bodnar spearheaded the COVID clinical care guidelines and order sets for non-ICU hospitalized patients within AgileMD, which are embedded into Epic and are being used across JHHS.
- Dr. Bimal Ashar stepped in to help Occupational Health set up their guidelines and testing and follow-up protocols, and what became the Employee Call Center.
- Dr. Stephen Sisson has established and overseen the CART which has fielded over 6,000 triage calls, and conducted over 1,000 follow-up remote clinical care encounters.
- Dr. Danielle Doberman has helped lead the Scarce Resource Committee as well as efforts to care compassionately for those dying in the hospital, including loosening of restrictions on visitors when appropriate.
- Nalynn Bellegarde, an NP on the Palliative team, coordinated a compassionate and thoughtful withdrawal of care for a patient in the CCU with 25+ family members in attendance via Zoom.
- Marylou Zyra, Caitlin McGeehan and Kristen Tweedy were redeployed to COVID units and assisted not only in the care of those patients, but by bringing their palliative skills to those areas. Marshall Gold and other were members of the Go Team, which assists with COVID-19 management in nursing facilities across Maryland.
- Dr. Joseph Cofrancesco and the IEE have created a new elective for medical students and multiple online sessions for faculty about how to teach using Zoom.
- Dr. Ashwini Davison has led a number of efforts for online education including a new MOOC on Telemedicine (w/Brian Hasselfeld, PT faculty, & Rebecca Canino), as well as helping the SOM transition to online learning for all the medical student courses.
- Dr. Amit Pahwa, who directs both the internal medicine and the pediatrics sub-internships, has developed new ways to keep the medical students engaged in patient care, but safely via Zoom.
- Dr. Richard Moore stood up and has chaired the Emergency IRB which meets daily to review COVID protocols. Dr. Mary Catherine Beach sits on this IRB as well.
- Dr. Lisa Cooper has spoken widely both internally and externally about how social inequities are playing a role in the COVID-19 pandemic and how this is impacting the most vulnerable in our communities. She was senior author of a paper in Annals of Internal Medicine with two GIM fellows, Drs. Lakshmi Krishnan and S. Michelle Ogunwole, on historical insights on the pandemic and racial disparities.
- Dr. Albert Wu has led the expansion of the RISE program for our employees, and has recommended (and published in Annals of Internal Medicine) three strategic principles for health care institutions responding to the pandemic.
- The Brancati Center has been accepting mask donations and delivering them to the community. They also started a newsletter to help our community members stay informed and safe.
- Dr. Joseph Cofrancesco, despite losing a brother to COVID at the start of the pandemic, has done three weeks of inpatient attending on the firms. For a video featuring Dr. Cofrancesco, visit: Johns Hopkins doctor on front lines lost brother to COVID, honors him by helping patients
For more COVID-19 photos, visit our Facebook page.
For more thank you posts, click here.
