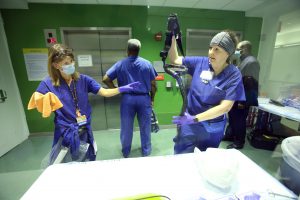
 No one is untouched by the COVID-19 pandemic. Although all departments in the School of Medicine and Johns Hopkins Health System have come together in remarkable ways to meet this challenge, no group has given more than the Department of Medicine. COVID-19 is fundamentally a medical illness, and our department is at the forefront in every aspect. Our nurses, residents, fellows, faculty and administrators are all involved and have substantially changed their work flow and, in many cases, their job descriptions to meet the demands of COVID-19. Each of our divisions has contributed in unique ways, addressing the clinical care, research and educational missions that are so critical to this response. With profound gratitude for these efforts, we are dedicating a series of brief reports to inform, thank and celebrate the contributions of these key divisions to our COVID-19 response.
No one is untouched by the COVID-19 pandemic. Although all departments in the School of Medicine and Johns Hopkins Health System have come together in remarkable ways to meet this challenge, no group has given more than the Department of Medicine. COVID-19 is fundamentally a medical illness, and our department is at the forefront in every aspect. Our nurses, residents, fellows, faculty and administrators are all involved and have substantially changed their work flow and, in many cases, their job descriptions to meet the demands of COVID-19. Each of our divisions has contributed in unique ways, addressing the clinical care, research and educational missions that are so critical to this response. With profound gratitude for these efforts, we are dedicating a series of brief reports to inform, thank and celebrate the contributions of these key divisions to our COVID-19 response.
Division of Endocrinology, Diabetes & Metabolism:
- The Division of Endocrinology, Diabetes & Metabolism hosts a town hall meeting every Friday. Faculty, staff and fellows hear the latest updates and ask questions in an open forum.
- At the start of the COVID-19 pandemic, the division sent daily email updates with important announcements affecting clinical, research, teaching and other operations. Recognizing the need for two-way communication (i.e. from leadership to clinicians/staff and vice versa) for open and timely dialogue, the division transitioned to Microsoft Teams as the main communication platform in early May. Our teams sites include 120 division members and partners from JHH, JHOC, BMC, GSS, GSS and Access Services. Since this communication platform was rolled out in early May, there has been a very high level of engagement, with 558 posts, 650 replies, 1,012 mentions and 324 reactions.
- They have also taken advantage of MS Stream to upload recorded lectures and grand round sessions to a teaching library on the Teams site.
- The division has taken full advantage of telemedicine and remote patient monitoring tools to manage patients with diabetes remotely. In fact, many patients have commented that the more frequent remote contact has allowed them to get better control of their diabetes care than they had been able to do so with less frequent in-person visits.
- Director Dr. Rex Ahima holds one-on-one and small group meetings with all faculty, staff and fellows to address concerns they may not feel comfortable expressing in the weekly townhall meetings.
- Nestoras Mathioudakis, Aniket Sidhaye, Misha Zilbermint, and Andrew Demidowich are involved in planning groups for a U01 multi-center RCT to evaluate whether intensive glycemic control improves outcomes in COVID-19.
- Adrian Dobs, director of the Johns Hopkins Clinical Research Network, has several research involvements related to COVID-19, including a large convalescent plasma study with Anne Arundel Medical Center and a vaccine study with Reading Hospital and Peninsula Regional Medical Center.
- Every member of the Division of Endocrinology, Diabetes & Metabolism has contributed in one way or another to ensuring that our patients received timely, compassionate, and expert endocrine and general medical care throughout the the pandemic.
- Endocrine faculty and fellows helped with the effort to cover inpatient medicine shifts. Nestoras Mathioudakis, Jenna Mammen, Amir Hamrahian, Justin Echouffo, Prasanna Santhanam, Aniket Sidhaye, Todd Brown, Suzanne Jan de Beur, Lediya Cheru, Daisy Duan (fellow), Kristen Jackson (fellow), Zach Simons (fellow), Colleen Gavigan (fellow), Leen Wehbeh (fellow), and Hasan Husni (fellow) collectively staffed 61 inpatient medicine day and overnight admitting and direct care shifts, totaling 531 hours. As many of our faculty and fellows had not recently done any inpatient general medicine work, a COVID-19 working group was formed with weekly team meetings where COVID-19 clinical management principles, inpatient logistics, and feedback was shared.
- Caitlin Nass, NP, Dr. Tom Donner, Dr. Sudipa Sarkar, Marybeth Carlin, RN and Dr. Nestoras Mathioudakis helped to quickly compile instructions for patients and providers to access a broad range of diabetes devices, including glucose meters, continuous glucose monitors, and insulin pumps. These instructions were converted into Epic smartphrases for our patients with video links, and provider instructions were placed on our division’s OneNote clinical resource manual. As our group was one of the first to put together a comprehensive set of diabetes patient data management instructions, these were shared nationally through the Epic endocrinology steering board.
- Endocrine faculty stepped up to precept our endocrinology fellows in one-on-one telemedicine sessions, which required that we significantly expand our pool of faculty preceptors. In addition, several faculty helped to fill gaps in our inpatient endocrine consult service that we created when division faculty had to assume inpatient medicine responsibilities.
- Division fellowship program leaders Dr. Roberto Salvatori and Dr. Kendall Moseley helped to quickly transition teaching conferences to a virtual forum, ensuring that the fellowship training continued uninterrupted.
- Endocrine nurses Marybeth Carlin, Deborah Dove, Adena Goldstein, Kathy Elza-Brown, Sally Snader and Sandra Ramsburg, transitioned from providing in-clinic to remote support of our patients and providers. Whether helping to clarify treatment plan, discussing clinical questions or medication side effects, assisting with prior authorizations, coordinating care with other specialists, or collecting diabetes data by phone, our compassionate and skilled nurses helped our patients to navigate a challenging medical system as smoothly as possible.
- The Endocrine Division moved its clinic location at Green Spring Station from the Joppa Concourse to Falls Concourse (Rockland Clinic), a space that is currently occupied by infectious disease. Adena Goldstein, RN, Paula Carter, CMA, and Kerry McNamara, PSC, took the lead on training new clinic staff on diabetes-related protocols, including point-of-care hemoglobin A1C testing and diabetes device downloads.
- Nestoras Mathioudakis, clinical director, helped to cover shifts in Occupational Health, the CART clinic, and the DOM Incident Command Center.
- Under the leadership of Dr. Aniket Sidhaye, director of the Inpatient Diabetes Management Service, our inpatient diabetes management service team (Holly Bashura, Anna Rendor, Rachhya Regmi, Erica Hall, Kimberly Vaughn, Asha Gullapalli) transitioned to virtual inpatient rounding, which allowed them to cover increased patient volumes during this period. Considering the association between diabetes and poor glycemic control with worse outcomes in COVID-19, the demand on our IDMS team was high during the covid peak at JHH and JHBMC.
- Dr. Rex Ahima, Dr. Sangwon Kim and Fred Anokye-Danso worked with the DOM and SOM to prepare the Endocrinology Research Labs at Bayview Medical Center for reopening.
- The endocrinology research labs at Bayview Medical Center hosts weekly virtual meetings for PIs, research staff, fellows and students to discuss papers and research advances.
- Douglass Montague, sr. administrative coordinator, came into the office every day to process mail and faxes to ensure clinical operations were not disrupted.
- The introduction of telemedicine outpatient clinics introduced complexity with clinical scheduling, particularly with assignments of faculty and fellows in primary vs. secondary provider roles. Lauren Pobletts, ambulatory service manager, undertook the herculean effort of transferring all the existing clinical schedules over to QGenda for a more streamlined scheduling process across all clinic locations.
- Medical Office Coordinators within the Division of Endocrinology – Alison Dimick, Myesha Eades, Tiffany Nesbitt, Kerry McNamara, Quoshay Thornton, Helen Bender, Muriel Jacobs, LaJoy Holmes, Sherene Fitzsimmons, Sharice Frazier, Kimberly Boyd - transitioned to working offsite while increasing their workload. In addition to their normal responsibilities, they have taken on active management of provider templates and rescheduling patients from in-person to telemedicine visits. Without their adaptability, the division would not have been as successful in meeting patient expectations.
- Ambulatory leaders and clinic managers at Endocrine clinics- Tammy Buettner, RN, Scott Goff, Ben Regalado, Gian Bonetti, Steve Roth, Deitra Rowlette, and Nicholas LaBricciosa helped to ensure that our patients and providers were safe during the ramp up to normal period as our clinics gradually reopened. This required careful consideration of room availability, endocrine clinical workflows, and HEIC protocols.
- Access Service specialists Manda Meadowcroft, Z Hearns, Noelle Davis, and Courtney Myles adjusted or created hundreds of clinic templates on incredibly short notice. At the start of COVID-19, the division developed a shared endocrine reschedule list in Epic that allowed our Medical Office Coordinators and providers to quickly indicate patients who needed to be rescheduled and to specify the visit type (in-person or video). Our Access Services team managed this list efficiently and accurately.
- Ambulatory clinic staff (CMAs/PSCs/RNs) at JHOC, JHBMC and GSS —Kim Neally, Roxanne Simon, Paula Carter, Aisha Burgess, Rhonda Austin, Patricia Patrick, Tonikeya Sykes, Deanna Carroll, Genevieve Vandespool, Taylor Scott, Holly Moss, Maryum Shadeed, Monay Dunmore, Myrtle Copeland, Mia Lacy, Latoria Merchant, Latonya Wiggins, Brittany Crum, Kathy Zmijewski, Kierra Hanley, Shymaeshia Jordan, Christopher Wheeler, LaToya Osborne and Cassandra Rookard adapted to supporting our clinicians remotely by going through the e-check in process. This real-time support dramatically increased the proportion of successfully completed telemedicine encounters.
- Research staff members Sonali Thapa, Smita Khati, Josh Garza and Alexis Page helped process information for the division during the initial COVID-19 transition and updated clinical calendars for all inpatient services.
Division of Hematology:
- Dr. Lanzkron, Dr. Pecker, PAC Mandy David, CRNP Ashley Lauriello, PAC Ijeoma Nnake, CRNP, Shannon Carroll and the rest of The Johns Hopkins Adult Sickle Cell Team have done an exceptional job in ensuring that care for adult sickle cell patients is not interrupted during this pandemic. The sickle cell clinic telemedicine visits actually increased the division’s outpatient volumes and is providing magnificent care.
- Dr. Streiff, pharmacist Peggy Krause and Claire Logue, BSN set up a seemless telemedicine anticoagulation program to manage patients on coumadin and other anticoagulants from afar.
- Drs. Strieff and Naik, with assistance from hematologic pharmacists Katie Dane and John Lindsley, established evidence-based COVID treatment/prophylaxis guidelines for across the institution for management of VTE.
- Inpatient heme4 service and Johns Hopkins Hematology-Oncology fellows took on extra shifts and provided inpatient guidance for clotting issues with COVID. Demand for these consults/curbsides was especially high in May and June.
- Dr. Naik almost single-handedly made the hematology GTS program the model for how to execute remote learning. The curriculum moved online in the middle of the heme course, but ratings from the students were outstanding and congratulatory.
- Drs. Chaturvedi, Braunstein and Naik each took numerous hospitalist shifts admitting COVID-19 patients, and the more senior hematology faculty backfilled their heme attending shifts in a true team effort to assist the Department of Medicine in demands to care for the surge of patients.
- Dr. Moliterno, Dr. Tara Robison and Janice Skinner coordinated complex telemedicine logistics for fellows clinic, JHOC and Bayview.
- Claire Logue, BSN, developed a Teams site for the division to provide faculty and staff with up-to-date information on the logistics of e-billing, telemedicine and e-consults.
- Dr. Resar received an internal JHU grant to study the role of HMGA-1 in COVID-19 disease.
- Divisional grants and research staff remotely coordinated complicated grants and research activities for various faculty including submitting COVID-19-specific clinical trials, despite tight deadlines.
- Office assistants and Medical Office Coordinators tirelessly aided in telemedicine and divisional scheduling.
For more COVID-19 photos, visit our Facebook page.
For more thank you posts, click here.
